|
12/28/2023 0 Comments Pediatric tidal volume calculatorWith the exception of children with obstructive pathophysiology, the physician should attempt to match the patient’s pre-intubation minute ventilation. Since pediatric respiratory rates vary wildly from adults, one should take the patient’s age into account when initiating mechanical ventilation (table 2). This should reassure the EP to choose their most familiar ventilator mode in conjunction with their intensivist. Despite all this complexity, there is a paucity of good evidence for or against any particular mode for ventilation the critically ill child. Pediatric patients are more likely than their adult counterparts to over-breathe the set respiratory rate, putting them at risk of breath stacking from large volume breaths. In SIMV, any time the patient initiates breaths within the set respiratory rate, a pressure supported breath (usually at 5-10 mmHg) is given rather than the full volume or pressure controlled breath. įinally, synchronized intermittent mandatory ventilation (SIMV) is often added to the above modes in pediatric ventilation. If the resulting tidal volume is too high, the next breath is delivered with less pressure, if the volume falls short of the targeted tidal volume, the next breath is delivered with more pressure (Table 1). With each breath the ventilator delivers a decelerating breath over the set time at an inspiratory pressure within the allowed range. The final commonly used mode for ventilating pediatric lungs is PRVC which, rather than requiring a set inspiratory flow rate like most volume controlled modes, utilizes a set inspiratory time, a targeted tidal volume, and a range of allowed pressures. This means that worsening compliance results in higher airway pressures (Table 1). The ventilator delivers a fixed flow of air until the desired tidal volume is reached. In contrast, VCV ventilation requires that the physician set the inspiratory rate, inspiratory flow rate, tidal volume, and PEEP. This means that worsening compliance results in low tidal volumes. When utilizing PCV, the provider sets the, inspiratory rate, inspiratory time, and inspiratory pressure meaning that the delivered tidal volume is dependent on the lung compliance of the patient. 
PCV is typically favored in neonates and infants while volume modes are preferred in larger children. The most commonly used modes for emergency pediatric ventilation include pressure assist control ventilation (PCV), volume control ventilation (VCV), and pressure regulated volume control ventilation (PRVC). Although the use of a Broselow tape and other height based methods of estimating body weight for drug dosing is fraught with error 5, the Broselow’s color coding allows for quick estimation of ideal body weight (IBW) that is required to calculate ideal tidal volumes.Īs mentioned, practice patterns related to pediatric ventilator management vary greatly. 
Like the Fat Man said in House of God: “ comes first.” The intubated child is bound for a pediatric ICU and hopefully the accepting pediatric intensivist is already aware of any intubated patient and can be a great deal of help and support as you work together to make your patient safe for transfer upstairs or across town. By keeping in mind small differences in pediatric physiology and keeping the consulting intensivist (and Broselow Tape) close at hand, an EP can effectively initiate mechanical ventilation in the smallest and most anxiety-provoking patients. However, pediatric ventilator management is largely driven by data extrapolated from adults, which should come as a relief to the EP. These unknowns can make the prospect of managing these patients even more intimidating. 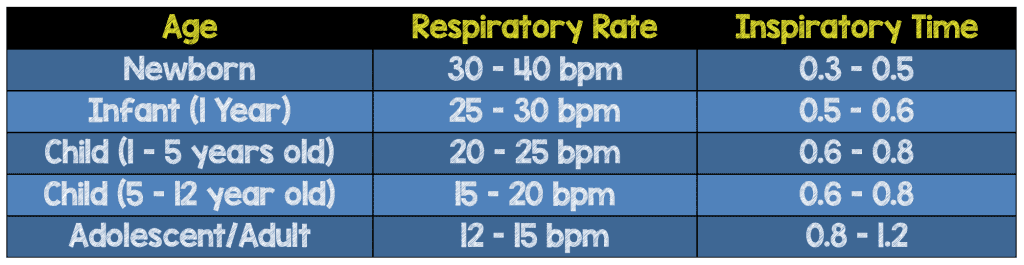
Additionally, evidence driven practice in pediatric mechanical ventilation is limited and practice patterns vary between institutions and providers. Hence, it stands to reason that EP experience with mechanically ventilated children can be scarce. Children are intubated three to six times less often than adult emergency department patients. Airway management of pediatric patients is a reasonable source of anxiety for the emergency physician.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
